Milk Proteins and Cardiovascular Health
Worldwide, cardiovascular disease is one of the leading causes of death. Preventing cardiovascular disease, through a healthy lifestyle and appropriate nutritional measures, is a public health issue. Dairy product consumption has repeatedly been correlated with cardiovascular disease risk in observational studies: the higher the consumption, the lower the risk.
In this respect, the role of proteins in milk, in particular caseins and whey proteins, has been extensively explored by scientists. The role of these proteins on three determinants of cardiovascular disease was explored: blood pressure, vascular function and lipid profile.
Milk Proteins and Blood Pressure
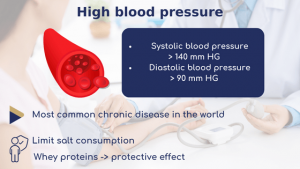
Arterial hypertension (AH) matches an abnormal increase in blood pressure on the artery walls, diagnosed when systolic and diastolic blood pressures exceed 140 mm Hg and 90 mm Hg respectively. It’s one of the key risk factors for cardiovascular disease, and the most common chronic illness in the world. From a nutritional point of view, limiting salt intake is considered the most effective measure for maintaining blood pressure at normal levels.
The protective link of certain dairy proteins against hypertension was suggested in the 1990s: in vitro and preclinical studies by Japanese researchers suggested the ability of certain dairy peptides to inhibit angiotensin-converting enzyme (ACE) [8, 9,10]. This enzyme is involved in the ability of arteries to contract, and therefore to promote hypertension. The dairy peptides involved, released after intestinal digestion, correspond to two specific sequences: valine-proline-proline (VPP), and isoleucine-proline-proline (IPP). A meta-analysis of these clinical trials found an average reduction in systolic blood pressure of -5.63 mm Hg, with supplementation durations ranging from 4 to 12 weeks [2]. Other meta-analyses, including a larger number of clinical studies, reach similar conclusion [6].
In addition to these studies testing the effect of peptides, the question is whether supplementation with milk proteins (caseins and whey proteins) produces similar effects. The experimental design remains identical in both studies, comparing the effects of whey protein, casein and maltodextrin (control condition), using a crossover experimental design allowing each volunteer to be his or her own control. In 2016, 38 volunteers took part in an initial study to assess the effect of the three conditions on blood pressure measured over a 24-hour period: only whey proteins managed to significantly lower systolic (- 3.9 mm Hg) and diastolic (- 2.5 mm Hg) blood pressure compared with the control condition [4]. In a second study, in 2018, the researchers this time gathered 27 volunteers to study the effect of the three experimental conditions on blood pressure in postprandial conditions: here again, whey proteins proved more effective than the other two conditions (caseins and maltodextrin) [5].
Milk Proteins and Vascular Function

Vascular function is closely linked to blood pressure, since it refers to the health of the arteries and their ability to dilate to regulate blood flow. A “flexible” artery will tend to be healthier than a “rigid” one, which will have more difficulty alternating dilation and constriction movements. In consequence, the results observed above can be explained by improvements in vascular function, and vice versa.
Here too, both peptides derived from milk proteins and milk proteins have been tested, sometimes in the same studies as those reported above. IPP and VPP peptides, supplemented in Japanese volunteers with mild hypertension for two weeks, significantly increased peak blood flow to several organs [7]. Some studies have also been carried out with the peptide NOP-47, derived from whey proteins: in volunteers without diagnosed hypertension, NOP-47 supplementation also improved arterial flow [1]. As no studies have directly compared the effects of casein peptides and whey protein peptides, it’s not possible to say whether some peptides are more effective than others; for the time being, all appear to have a positive effect on vascular function.
A few clinical studies have also been carried out with milk proteins. Agnès Fekete’s research group directly compared the effect of caseins and whey proteins on vascular function, in “normal” and post-prandial situations. In a “normal” physiological situation, in patients with hypertension, caseins and whey proteins do equally well, significantly improving arterial flow compared with the control condition [4]. In postprandial conditions, however, whey proteins stand out as the only ones to improve arterial flow [5]. Interestingly, this improvement correlates with lower blood pressure for whey proteins, but not for caseins: suggesting different mechanisms of action for the two proteins.
Milk Proteins and Lipid Profile
The lipid profile is another cardiovascular risk parameter, and generally matches the study of circulating cholesterol levels (total cholesterol, HDL cholesterol and LDL cholesterol), as well as the study of plasma triglyceride concentrations. Research work concurs on the need to monitor concentrations of these criteria, to prevent the risk of cardiovascular disease. As far as lipid profiles are concerned, dairy proteins (caseins and whey proteins) have been exclusively studied to date; the effect of peptides derived from these proteins has not been directly explored, and is therefore unknown to date.

Several of the studies cited above can be found in this section, the authors having also measured the impact of given supplements on lipid profile. For example, a study of whey protein or casein supplementation in people with mild hypertension showed a significant reduction in circulating total cholesterol; only whey protein, on the other hand, was able to significantly lower circulating triglyceride levels in the study [4]. Concordantly, other researchers have found a similar effect of whey protein in overweight or obese people: significant reductions in circulating levels of total cholesterol, LDL cholesterol and circulating triglycerides [11].
Several mechanisms of action are considered to explain these benefits, recorded for caseins but especially for whey proteins. As for caseins, several researchers have raised the issue of their high calcium content, which they believe is capable of combining with fatty acids and bile acids to form insoluble compounds that cannot be absorbed and are therefore eliminated by the body, potentially explaining the drop in circulating triglycerides [12]. In the case of whey proteins, however, it’s the high content of branched-chain amino acids (BCAAs) that could be the key: these amino acids are involved in the intestinal absorption of fatty acids and cholesterol, which could explain the clinically observed drop in these parameters [3].
Conclusion
The physiological effect of milk proteins on cardiovascular function is relatively unknown, as milk proteins are generally associated with other types of physiological benefits, such as satiety, muscle mass synthesis and keeping blood sugar levels within the normal range. However, a large body of research, including clinical studies, suggests that these proteins have physiological benefits for the cardiovascular system at three levels: blood pressure, vascular function and lipid profile.
The effects on blood pressure and vascular function are physiologically very similar, and are probably the most convincing, given the number of clinical trials conducted on both proteins and peptides derived from these proteins. The impact of milk proteins (caseins and whey proteins) on the lipid profile is less well explored, but the results of clinical trials are promising. Taken together, these results may explain the protective association between dairy consumption and cardiovascular disease risk. Finally, clinical studies that have resorted to pure protein supplementation also suggest that these proteins have an impact regardless of their original matrix, and as such can be incorporated into a wide range of foods to take up their physiological effects.
Sources:
[1] Ballard, K. D., Bruno, R. S., Seip, R. L., Quann, E. E., Volk, B. M., Freidenreich, D. J., Kawiecki, D., Kupchak, B. R., Chung, M., Kraemer, W. J., & Volek, J. S. (2009). Acute ingestion of a novel whey-derived peptide improves vascular endothelial responses in healthy individuals: a randomised, placebo-controlled trial. Nutrition Journal, 8(1). https://doi.org/10.1186/1475-2891-8-34
[2] Chanson-Rolle, A., Aubin, F., Braesco, V., Hamasaki, T., & Kitakaze, M. (2015). Influence of the lactotripeptides Isoleucine-Proline-Proline and Valine-Proline-Proline on systolic blood pressure in Japanese subjects: A Systematic Review and Meta-Analysis of Randomised Controlled Trials. PLOS ONE, 10(11), e0142235. https://doi.org/10.1371/journal.pone.0142235
[3] Chen, Q., & Reimer, R. A. (2009). Dairy protein and leucine alter GLP-1 release and mRNA of genes involved in intestinal lipid metabolism in vitro. Nutrition, 25(3), 340-349. https://doi.org/10.1016/j.nut.2008.08.012
[4] Fekete, A., Giromini, C., Chatzidiakou, Y., Givens, D., & Lovegrove, J. A. (2016). Whey protein lowers blood pressure and improves endothelial function and lipid biomarkers in adults with prehypertension and mild hypertension: results from the chronic Whey2Go randomised controlled trial. The American Journal of Clinical Nutrition, 104(6), 1534-1544. https://doi.org/10.3945/ajcn.116.137919
[5] Fekete, A., Giromini, C., Chatzidiakou, Y., Givens, D., & Lovegrove, J. A. (2018). Whey protein lowers systolic blood pressure and Ca-caseinate reduces serum TAG after a high-fat meal in mildly hypertensive adults. Scientific Reports, 8(1). https://doi.org/10.1038/s41598-018-23333-2
[6] Fekete, A., Givens, D., & Lovegrove, J. A. (2015). Casein-Derived lactotripeptides reduce systolic and diastolic blood pressure in a Meta-Analysis of randomised clinical trials. Nutrients, 7(1), 659-681. https://doi.org/10.3390/nu7010659
[7] Hirota, T., Ohki, K., Kawagishi, R., Kajimoto, Y., Mizuno, S., Nakamura, Y., & Kitakaze, M. (2007). Casein hydrolysate containing the antihypertensive-tripeptide Val-Pro-Pro and Ile-Pro-Pro improves vascular endothelial function independent of blood Pressure-Lowering effects: contribution of the inhibitory action of Angiotensin-Converting enzyme. Hypertension Research, 30(6), 489-496. https://doi.org/10.1291/hypres.30.489
[8] Masuda, O., Nakamura, Y., & Takano, T. (1996). Antihypertensive Peptides Are Present in Aorta after Oral Administration of Sour Milk Containing These Peptides to Spontaneously Hypertensive Rats. Journal of Nutrition, 126(12), 3063-3068. https://doi.org/10.1093/jn/126.12.3063
[9] Nakamura, Y., Masuda, O., & Takano, T. (1996). Decrease of Tissue Angiotensin I-Converting Enzyme Activity upon Feeding Sour Milk in Spontaneously Hypertensive Rats. Bioscience, Biotechnology, and Biochemistry, 60(3), 488-489. https://doi.org/10.1271/bbb.60.488
[10] Nakamura, Y., Yamamoto, N., Sakai, K., Okubo, A., Yamazaki, S., & Takano, T. (1995). Purification and Characterisation of Angiotensin I-Converting Enzyme Inhibitors from Sour Milk. Journal of Dairy Science, 78(4), 777-783. https://doi.org/10.3168/jds.s0022-0302(95)76689-9
[11] Pal, S., Ellis, V., & Dhaliwal, S. S. (2010). Effects of whey protein isolate on body composition, lipids, insulin and glucose in overweight and obese individuals. British Journal of Nutrition, 104(5), 716-723. https://doi.org/10.1017/s0007114510000991
[12] Thorning, T. K., Bertram, H. C., Bonjour, J., De Groot, L. C. P. G. M., Dupont, D., Feeney, E. L., Ipsen, R., Lecerf, J., Mackie, A., McKinley, M., Michalski, M., Rémond, D., Risérus, U., Soedamah-Muthu, S. S., Tholstrup, T., Weaver, C. M., Astrup, A., & Givens, I. (2017). Whole dairy matrix or single nutrients in assessment of health effects: current evidence and knowledge gaps. The American Journal of Clinical Nutrition, 105(5), 1033-1045. https://doi.org/10.3945/ajcn.116.151548